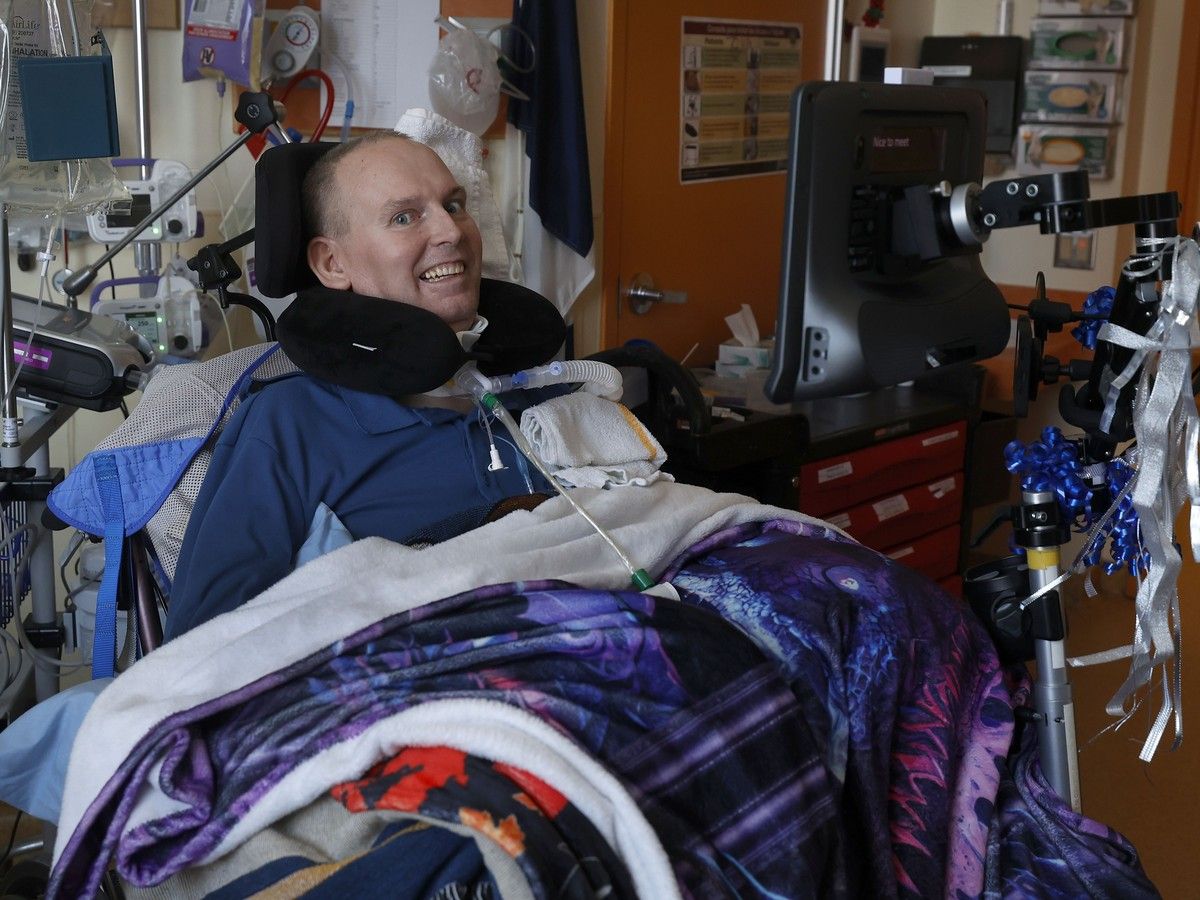
On a late winter day, the sun seeped into Andrew Chernysh’s room inside Ottawa’s century old
Saint-Vincent Hospital
. It illuminated family photos and postcard-sized Group of Seven prints that blanket one wall and bounced off a bouquet of birthday balloons suspended near his wheelchair.
The military veteran and cybersecurity specialist smiled.
Chernysh, 52, has advanced ALS (
amyotrophic lateral sclerosis
). He was diagnosed with the neurodegenerative disease five years ago. He is paralyzed from the neck down and is fully dependent on others for his needs. He relies on a ventilator to breathe.
A career computer guy, Chernysh communicates by using his eyes to spell words on a computer fitted with eye-gaze technology. The computer spells out each letter, each word and then the whole sentence. During an interview, Chernysh looked up and smiled at the end of each computer-voiced sentence.
He only expected to live a year after entering the palliative care program for patients with complex health needs at Bruyère Health’s Saint-Vincent Hospital. That was in 2024.
Like many palliative patients, Chernysh was struggling with severe psychological distress. It is something up to half of patients with advanced illness experience as they approach end of life.
He had signed a waiver of consent for medical assistance in dying (MAID) and was seriously considering it.
Today, he continues to look to the future. When asked whether he is happy, his eyes spell out Y-E-A-H on the computer. “I enjoy the simple things — the sun and visitors and activities,” he adds, speaking through the computer.
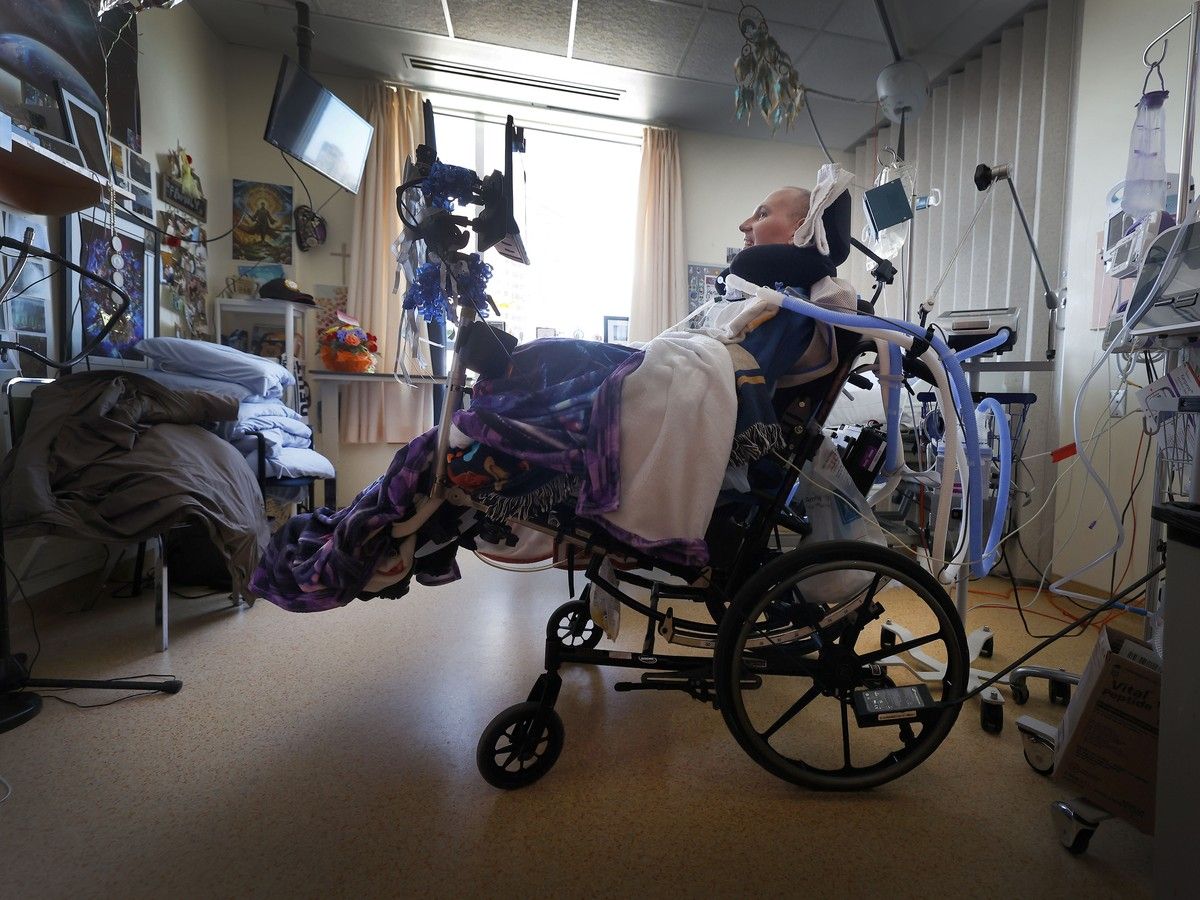
Chernysh is part of a novel research trial — the first of its kind — using microdoses of psilocybin to treat palliative patients experiencing severe psychological distress. The aim of the research is to see whether small doses of the psychedelic medication can help manage symptoms and alleviate depression, anxiety and existential distress.
Lead author Dr. James Downar, a palliative physician at Ottawa’s Bruyère Health and senior investigator at the
Bruyère
Health Research Institute, says severe psychological distress in palliative patients is both common and difficult to treat. Standard medications to treat symptoms such as anxiety and depression take time that palliative patients don’t have.
“We really don’t have particularly effective, scalable therapies for this.”
He notes that giving patients with severe psychological distress more assistance and support misunderstands the nature of the condition. “It is not caused by the fact that they can’t get help. It is caused by the fact that they need it. They do not want people to help them. They want to be able to do it on their own.”
Chernysh was one of 20 patients who took part in a preliminary study looking into the safety and efficacy of the treatment.
In a recently published paper in the journal Palliative Medicine, researchers reported that a majority of those in the trial felt they had “meaningful improvement” over the three-week trial. That includes 72 per cent who had improved “demoralization scores” — measured by loss of meaning and purpose, distress and coping abilities. Sixty-two per cent reported a more than 50 per cent improvement in measures of depression. There were no serious adverse effects among participants.
Downar says there has long been anecdotal talk about the positive impact of microdoses of psilocybin, but it has not been well studied because the drug is not legal.
Research using psilocybin, the psychedelic ingredient in magic mushrooms, is undergoing a resurgence. It has been used effectively in a highly supervised form of mental health treatment that combines psilocybin with traditional psychotherapy. Psilocybin is illegal in Canada but special access is allowed in some cases for its use in psychotherapy and for research.
Subjects in the Bruyère study took microdoses a couple of times a week — “just the way you might take Aspirin,” according to Downar. Unlike the drug’s use in other therapies, patients taking microdoses do not experience any psychedelic effects, he said.

Downar called the early results exciting and said he is cautiously optimistic, although more research needs to be done to draw conclusions about the drug’s effectiveness. He is starting a larger, randomized control trial to get answers about whether the treatment shows benefits and could be used on a larger scale to treat patients. If so, it would fill a “really important gap in our tool box to treat this kind of distress.”
Downar says some of the participants in the early research have reported just feeling better overall, sleeping better and being better able to focus and control their thoughts.
Chernysh said that he became less anxious almost immediately after starting to take the microdoses of psilicyban and that symptom relief had continued. As a result, he said, he is more interested in taking part in activities available and feels better.
He was keen to talk about the positive impact of the treatment on his quality of life.
Earlier in the week, some friends he has known since his days at Royal Canadian Military College stopped by to help Chernysh celebrate his 52 birthday. Hanging prominently on his wall of photos and art is a grad picture of him dressed in a scarlet tunic.
The computer is Chernysh’s lifeline. He keeps in touch with friends and family, is active on social media and can order things — postcards of Group of Seven paintings and computer gadgets and more — from Amazon. He can also play some computer games.
He calls eye-gaze technology, which allows him to communicate in person and online, “awesome.”
During an interview in his hospital room, Chernysh talked about his hope that he might benefit from more technology as part of a clinical trial involving implanting a chip into the brain to help patients with paralysis control a robotic arm with signals from their brains.
That is not confirmed, but Chernysh is hopeful.
“Maybe,” he says, while talking about the possibility.
Downar says he enjoys visiting Chernysh to administer medication as part of the trial.
“It is a joy to see this person every day. It is kind of fun when you see how much this person is not in distress. It is very rewarding.”
The treatment, Downar says, is not about avoiding MAID “it is just about making people feel a little bit better for whatever time they have.”
Chernysh smiles throughout an interview about the clinical trial.
“I try to be optimistic,” he says.
Related
- Refugee and immigrant children less likely to go to hospital emergency for minor ailments: study
- What happens when youth, even children, are tasked as caregivers?
Our website is your destination for up-to-the-minute news, so make sure to bookmark our homepage and sign up for our newsletters so we can keep you informed.